‘Secondhand chemo’ puts healthcare workers at risk
Sue Crump braced as the chemo drugs dripped into her body. She knew treatment would be rough. She had seen its signature countless times in the ravaged bodies and hopeful faces of cancer patients in hospitals where she had spent 23 years mixing chemo as a pharmacist.
At the same time, though, she wondered whether those same drugs – experienced as a form of “secondhand chemo” — may have caused her own cancer.
Chemo is poison by design. It’s descended from deadly mustard gas first used against soldiers in World War I. Now it’s deployed to stop the advance of cancer.
Crump knew she had her own war on her hands. She wanted to live long enough to see her 21-year-old daughter, Chelsea, graduate college.
And she wanted something else: She wanted young pharmacists and nurses to pay attention to her story.
Crump, who died of pancreatic cancer in September at age 55, was one of thousands of health care workers who were chronically exposed to chemotherapy agents on the job for years before there were even voluntary safety guidelines in place.
Now some of those workers are being diagnosed with cancers that occupational health specialists say could be linked to exposure to the same powerful drugs that have saved hundreds of thousands of patient lives. Experts believe that’s because when nurses, pharmacists, technicians and increasingly, even veterinarians, mix and deliver chemo, accidental spills, sprays and punctures put them in close, frequent contact with hazardous drugs.
Yet an InvestigateWest investigation has found that the federal Occupational Safety and Health Administration does not regulate exposure to these toxins in the workplace, despite multiple studies documenting ongoing contamination and exposures. Studies as far back as the 1970s have linked increased rates of certain cancers to nurses and physicians.
Exposures continue to occur. A just-completed study from the U.S. Centers for Disease Control, 10 years in the making and the largest to date, confirms that chemo continues to contaminate the work spaces where it’s used, and in some cases is still being found in the urine of those who handle it, despite knowledge of safety precautions.
Chemo agents have been classified as hazardous by the Occupational Safety and Health Administration (OSHA.)since the mid-1980s.Hazardous drugs are those known, or suspected to cause cancer, miscarriages, birth defects, or other serious health consequences.
Deputy Assistant Secretary of Labor for OSHA Jordan Barab said in written response to questions from InvestigateWest that the agency doesn’t have resources to regulate workplace drug exposures, although it is concerned about the issue. “Although this is an important safety and health issue, OSHA has not considered a standard to specifically address hazardous drugs in the healthcare setting,” he wrote.
OSHA has no regulatory authority to enforce safety practices with fines or sanctions, other than under its “General Duty” clause – a catch-all regulation that allows OSHA inspectors to warn an employer if they see something that concerns them.
According to documents obtained by InvestigateWest through the Freedom of Information Act, OSHA has only used the General Duty Clause once in 10 years to cite any health care institution, including hospitals, clinics, dental and veterinary offices, for their handling of hazardous drugs.
In contrast, there are enforceable standards, including “permissible exposure limits” to protect workers from other known cancer-causing hazards, such as benzene, or asbestos. The government also has standards for healthcare workers handling radiation and certain chemicals, such as sterilizing agents.
But not for drugs.
“There is no other occupation population (that handles) so many known human carcinogens,” said Thomas Connor, a research biologist with the National Institute for Occupational Safety and Health. Connor has spent 40 years studying the effect of chemo agents on workers, and is one of the lead authors on the latest study.
Tracing an individual’s cancer to a particular exposure is difficult. It’s one of the main reasons safety advocates have been thwarted in their efforts to get stricter regulations. But the ranks of those who have became symbols for increased safety includes pharmacists Bruce Harrison of St. Louis and Karen Lewis of Baltimore, veterinarian Brett Cordes of Scottsdale, and nurse Sally Giles of Vancouver, B.C.
All of them eventually got cancer, or in Lewis’ case, a pre-cancerous condition. Cordes was diagnosed four years ago at age 35. Giles was in her 40s, and Lewis and Harrison were in their 50s when diagnosed. All but Lewis and Cordes are now dead.
Sue Crump’s war
On an afternoon in May of 2009, Crump sat in a coffee shop near her Redmond home, and perused a list of chemo drugs now deemed hazardous for healthcare workers to handle. She runs her fingers down the page. It’s a long list: cyclophosphamide, doxorubicin, fluorouracil, methotrexate. And the list went on.
“Yeah, I worked with all of them,” she said.
Crump is there with her daughter, a journalism student at Western Washington University. They share the same hazel eyes, light brown hair and dry sense of humor. They’re both talkers, but her mother, according to Chelsea Crump, can outtalk even her. They finish each other’s sentences in the way mothers and daughters have for generations.
“Chemo brain” has slowed her mom down only slightly, Chelsea joked.
Sue Crump followed an older cousin into the pharmacy profession. It suited her. She was meticulous, independent, and good with math. She liked being part of a helping profession, and enjoyed her occasional contact with patients.
Mostly, though, she was a mixer.
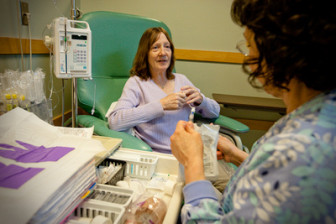 Crump started at Swedish Medical Center in the early 1980s, before pharmacists used special protective “hoods” over countertops to contain spray and chemo contamination. They didn’t use gowns, or gloves.
Crump started at Swedish Medical Center in the early 1980s, before pharmacists used special protective “hoods” over countertops to contain spray and chemo contamination. They didn’t use gowns, or gloves.
They had no reason to think they should.She even brought Chelsea – then a toddler – to work with her.
“I would play with a bucket of water, and the syringes,” said Chelsea.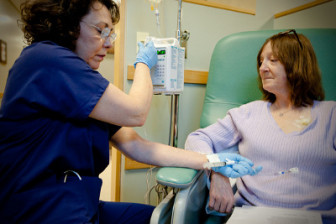
Occasionally, drugs would spill on the countertops.
“We would wipe if off and throw (the towels) in the garbage,” said Sue Crump.
Most of the chemo came in vials, and they would transfer it into plastic IV bags. Sometimes there would be spray when they punctured the vials.
Other drugs came in ampoules, small, sealed glass vessels ready for a single infusion. “I’d file the neck of it, then snap real fast, she said. “A lot of times, I got cuts.
“But the feeling at the time was – whatever little vapors or splash – it was such a low exposure through the skin, it was insignificant.”
That was a common attitude then – and now, said Dr. Melissa McDiarmid, director of occupational health at the University of Maryland in Baltimore.
“So many people think it’s just a ‘little bit.’ They don’t understand, it’s a little bit of something designed to be toxic, and to be highly absorbed biologically.”
A silent threat
Chemotherapy agents, when dispersed in the air, or onto surfaces, are invisible, difficult to clean, long-lasting, easily spread, and capable of causing genetic damage. They’ve been found on the outsides of the drug vials shipped from manufactures, on floors and countertops, on keyboards, and garbage cans, and door knobs.
“Cytoxan (cyclophosphamide) is one of the worst drugs out there, and one of the most common,” said Marty Polovich, associate director of the Duke Oncology Network at Duke University, who has been working to strengthen and refine guidelines for more than 20 years.
“It has good staying power,” she said. “There was spill on a floor in a pharmacy, and eight months later, they still found it.”
Seth Eisenberg, an oncology nurse for the Seattle Cancer Care Alliance, who also speaks nationally to nurses about safety issues, calls contamination of workplaces a “double whammy.”
“It’s difficult to detect,” he said. “And difficult to get rid of.”
The union that represents nurses nationally is worried, too.
“It’s been a silent threat for a long time with very little attention by the government,” said Bill Borwegen, occupational health and safety director for the Service Employees International Union, the labor union that represents nurses nationally.
“We are concerned how they are handled. There’s such a dearth of info on how to sample these agents. People don’t know how to clean surfaces.”
Cancer has a long latency period, and its genesis is complex, likely a combination of environmental exposures and hereditary tendencies.
“Most of the chemo agents are genotoxic,” said Connor. They interact with DNA, causing mutations. Genetic mutations, in turn, are a known risk factor for developing cancer. And secondary cancers, especially of the blood or bladder, are a known side effect of treatment for cancer.
Unlike some European countries, however, the U.S. does not have good tracking mechanisms to link occupational exposures to subsequent cancers.
“No one is really following these people to see – are they dying?” Connor said. “No one is following this in a systematic, effective way.”
Danish epidemiologists used cancer registry data from the 1940s through the late 1980s to report, beginning in 1975, a significantly increased risk of leukemia among oncology nurses and later physicians.Last year, another Danish study of more than 92,000 nurses found an elevated risk for breast, thyroid, nervous system and brain cancers in the nursing population.
In the U.S., a sprinkling of anecdotal case studies in the medical literature also pointed to the potential health consequences. In 1993, for example, there was a published case detailing the exposure and subsequent cancer developed by a 39-year-old female pharmacist. Twelve years earlier, the “non-smoking, vegetarian” pharmacist had worked preparing daily doses of commonly used chemo drugs, including cyclophosphamide, fluorouracil, methotrexate, doxorubicin, and cisplatin. She used the type of hood that was later shown to blow air from the back of the hood, over the drugs, and out the opening into the environment where she stood. According to a summary of the paper: “Except for preparing (chemo drugs,) no other risk factors for bladder cancer could be identified. Because bladder cancer occurs predominantly in older white men and in cigarette smokers, this case is particularly noteworthy.”
Researchers at NIOSH, a division of the CDC, were so concerned by mounting evidence, they issued an extensive alert about handling high-risk drugs. The guidelines, published in 2004, urge strict precautions, including use of impervious chemo gowns, double-gloving, use of sophisticated “closed-system” devices and specialized ventilation hoods, face shields and respirators, clean rooms, and other precautions.
But the NIOSH guidelines outlined in the alert are voluntary.
That’s wrong, said McDiarmid. “We can no longer have these be optional. We’re talking human carcinogens here.”
‘Welcome to the club’
Ten years into Crump’s career, reports of health effects related to chemo exposure began to surface in Europe and healthcare workers started adopting rudimentary safety procedures.
Her pharmacy manager at Swedish took the warnings seriously and installed special ventilated hoods in the workspaces – considered state-of-the-art at the time.
The trouble was the hoods were designed to keep chemicals sterile by blowing contaminants away from them and back out of the hood. That meant the worker standing outside the hood was still getting exposed, Crump said.
Lanny Turay worked in the same pharmacy as Crump and recalled many of the same experiences. He now manages pharmacy operations at Swedish Cancer Institute.
Safety practices have evolved over the years. Swedish now has a special dedicated area for mixing chemo, and uses a different type of hood that no longer blows air back at the workers. Workers wear special gowns, gloves and sleeves, and take other precautions to keep chemo from spreading around, he said.
 Still, Crump wondered whether those early, ongoing exposures had contributed to the cancers she and her peers have gotten. She first recalled getting alarmed after a pharmacy tech – someone with whom she mixed a lot of chemo — died at age 29 of a brain tumor. Around the same time, several colleagues experienced miscarriages.
Still, Crump wondered whether those early, ongoing exposures had contributed to the cancers she and her peers have gotten. She first recalled getting alarmed after a pharmacy tech – someone with whom she mixed a lot of chemo — died at age 29 of a brain tumor. Around the same time, several colleagues experienced miscarriages.
Since that time, a number of studies have shown an association between exposure to chemo agents and adverse reproductive effects including miscarriage, birth defects and low birth weights. A 2005 survey found significant associations with infertility and miscarriage in nurses who handled chemo before the age of 25. Nurses, who occasionally spill the chemo drugs on their clothing or splash it on their skin, had a greater chance of premature labor if they mixed nine or more doses a day. Having children with learning disabilities was associated with how frequently their mothers wore gloves while handling chemo.
“Now all these people about my age are getting cancer – cervical, ovarian, prostrate, endometrial, brain,” Crump said. “All of us, at one time or another, worked with chemo – we wondered, well, is there a connection?”
Chelsea Crump recalled her mother’s cousin, her boss, her best friend – all worked with chemo. All got some form of cancer.
When her mother called to inform one friend about her cancer, the friend, who was also a pharmacist and also a cancer patient, said, “Welcome to the club.”
‘Chemo roulette’
Safety advocates are especially worried about workers in smaller clinics, where awareness may not be as high as at large cancer centers, and where expensive equipment may be less available.
There are more than 5.5 million workers involved in nursing, pharmacy, transport and cleanup of chemo waste. Of those, experts estimate about 2 million actually mix or dispense chemo. It can be a messy job. McDiarmid, the occupational health expert, got interested in the field after she saw a nurse spill the contents of a bottle of chemo drugs on herself and become violently ill.
Those numbers will grow as the ranks of cancer patients climb by a projected 50 percent in the next decade as the population ages. More people will be required to prepare and deliver their treatment. And more of those people will likely be in non-hospital settings such as outpatient clinics, or private homes.
“Home health is a mess,” said McDiarmid. Drugs are mixed at home health pharmacies and put in zip lock bags and sent off to the home, she said. “Where the wheels come off is in the home itself – there are no regulations about where to dump bedpans or trash.”
In addition, chemo drugs themselves have found wider application – in the treatment of arthritis, multiple sclerosis and other diseases – which puts them in a wider array of physicians’ offices.
And veterinarians are now increasingly using these drugs to treat animals, putting those who work in vet’s offices in contact with chemo.
Generic drugs have made the treatment more affordable for pet owners, said Cordes, the vet who became a safety consultant after he was diagnosed with thyroid cancer. Cordes said he, like many vets he’s spoken with, handled chemo without understanding its dangers. More safety info is made available to practitioners of human medicine, he said. “We slip through the cracks.”
Luci Power, former senior pharmacy manager at University of California San Francisco Medical Center, was one of the first to blow the whistle on unsafe practices in the early 1980s. Power continues to advise professional groups about safety practices, and she said denial continues to be a huge problem.
“They want to know the body count. To them this is all theoretical and scare tactics. They don’t really believe us,” she said. “Without numbers, people just choose not to think it can hurt them.”
This lack of data has created a giant Catch-22 for those advocating safer workplaces. Many employers – and workers themselves — simply don’t view this as a problem, and push back against the hassle of expensive, time-consuming changes that would protect workers from exposure.
“Nurses say, ‘well, we don’t like wearing gloves and gowns – we don’t want to scare the patients,’ ” Power said.
Anecdotally, many accounts suggest there is widespread variability in safety practices, that gowns and gloves are re-used, and that even existing safety protocols may be inadequate to prevent contamination.
In 1999, Connor and others published a paper showing surface contamination in six hospitals in North America. The pharmacies were using “biological safety cabinets,” – specialized chemo hoods that are supposed to stop contamination — but the study showed the drugs were still not contained.
“People thought that was a magic box,” he said. “But once you put your arms in there, it breaks the seal. And they’re packing them full of equipment – taking things in and out. People’s hands are contaminated, (their) gloves, badges.”
“Gown use is terrible – it’s not improved in 20 years,” said Polovich.
Eisenberg, the safety expert, said in his experience, gowns are only used about 50 percent of the time they are recommended. He calls this cavalier attitude toward worker safety, “chemo roulette.”
People don’t take this seriously enough
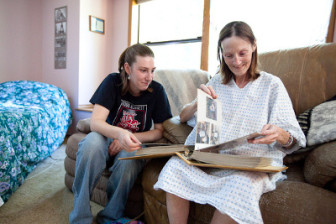 On a sunny day in June 2009, Sue Crump has a list of things to do.
On a sunny day in June 2009, Sue Crump has a list of things to do.
She needs to teach Chelsea about mortgages, and schedule an appointment with a financial planner. They are going through boxes of old photographs.
“I’m a practical thinker,” she said. “And I’m practical about this.”
Pancreatic cancer carries a grim prognosis. By the time it’s diagnosed, it’s typically too late to cure.
At first, she thought her symptoms – weight loss, gastro-intestinal distress, fatigue — were related to the divorce she was going through at the time. She thought the stress was giving her an ulcer.
She had taken a break from pharmacy and had taken a job as a tax-preparer. A week before tax season ended, she learned she had a large tumor in her abdomen.
Crump has already outlived various prognoses – 3 to 6 months, then 6 months to a year. It’s been over a year now. Crump attributes it to sheer orneriness.
“I’m Scotch and Irish,” she said. “My Dad always said I’m two kinds of stubborn.”
But cancer is a leveler, and her tumor markers are on the march. They’ve quadrupled in a few months.
She can only tolerate soup, Jell-O and cottage cheese. She’s been trying to prepare her whole family for what she knows will come.
By last fall, the cancer was on its final assault.
Chelsea Crump took a semester off from school to take care of her mom through her final illness. Chelsea nursed her mother in the Redmond house her mother built, on land Sue Crump bought and cleared herself before she got married.
Together they managed to squeeze in a few last life-list goals – visiting Disney World for the first time, and seeing the famous Lipizzaner white stallions perform. They spent time running her beloved dogs up on some woodland property she loved.
Crump joked she wanted her soccer-playing daughter to “drop-kick me in the river” up there when it came time to put her remains to rest.
She could still make her daughter laugh.
Sue Crump was stubborn to the end, cheating her expected death several times, before finally succumbing, surrounded by her family and her beloved dogs, in her own living room on September 13.
Shortly before she died, she said she hoped talking about her experiences would make a new health care worker pay a little more attention.
“Safety needs to be revisited,” she said. “People don’t take this seriously enough.”
And she extracted a promise from her daughter.
Just before her mother died, Chelsea Crump promised her she would go back to school and finish the degree in journalism that she had started.
She also promised she would share her mother’s story.
Read more about this story.



So, according to the Occupational Safety and Health Administration (OSHA.), chemotherapy drugs are
hazardous and known to cause cancer, miscarriages, birth defects, or other serious health problems. So why are they used to treat cancer. You cannot cure cancer with a substance that causes cancer. The idea that you can is illogical.
This story is very sad. Of course they don’t know why she got cancer and it may or may not be the result of handling chemotherapy agents for so many years without proper safeguards. We’ll probably never know We have no idea why my mother, with no known risk factors, succumbed to uterine cancer last year. I agree, chemotherapy drugs are toxic carcinogenics. Surely there has to be a better way to try to fight cancer.
I have several markers in family history for cancer. Drs are watching for colon, anal, stomachache an thyroid cancer. My work is now making me make chemo again again. I feel this is a death sentence. I have seen miscarriages RPh;s are now getting cancer that is not family related. Now they management are having techs make chemo. The are not being trained in all the safety . I am being forced to make chemo again with all my family risk factors. This js just greed bastards using techs that don’t know the dangers of what they are doing. I am trying to get a waiver from one of my Drs so I don’t have to make this stuff. I already did this for 2 yrs in a row every day and got out because I was getting sick. I was tasting matalic taste. WE had at the time a closed system where 1% of the chemo was coming aback into the room.That has changed but I don’t want to take the risk. I have seen 3 RPHS get breast cancer where here was no family history of markers. They were all in there late 40’s early 50’s. Common sense tells me there were out side sources working. I have know RP h that are going to die from the cancer they receive making it back in the 80’s where were less precautions than there is now. I don’t think any one should be forced to do this work just because the job description was rewritten to include you make you do this. We should have freedom of choice of choice this is our bodies and life we are talking about. But the almighty dollar is dictating what we can do with our bodies. That is wrong.
I have seen an increase of early miscarriage iin the IV room. we do not have a separate room for making chemo.
Why is chemotherapy used? Profit, it makes money for Big Pharma and your local, oncologist. He (she) makes money on every vial of the poison they sell. In fact, up to 75% of an oncologist’s income comes from the profit on the poisons they pump into patients! http://www.nytimes.com/2010/06/17/health/17drug.html
Bottom line: How many cancer docs would take chemo or reecommend it to family members if they had cancer? Out of 64 oncologists surveyed, 58 said…http://diabetic-test-strips.blogspot.com/2009/12/91-of-canccer-docs-wont-take.html
Bill Young, Alternative Nutrition Therapist
This story is so sad. I have never posted a comment anywhere before but this takes the cake. First I pray for God’s peace and comfort for this family—-it sounds as if there are pretty tough genes in this family. Something that concerns me about this article is “When nurses or doctors know what they know about the chemo drugs, how can they think it’s healing -not to mention life threatning to inject someone.” I have lost several people close to me from cancer and don’t understand why ignorance in the “Let’s treat cancer with poison” case is justifiable. ————–Oh-I guess I do understand it it is GREED. Not only should chemo drugs be regulated by OSHA the doctors who prescribe it should be also. It seems to me that is like blaming the guns for killing people and not the person shooting them.