Oregon families of medically fragile children grapple with uncertain future of longtime Providence center
By Kaylee Tornay / InvestigateWest
June Stracener’s bedroom would be like any other teenager’s — Taylor Swift playing, a cloud lamp overhead and colorful art on her wall — if not for the medical devices around her hospital bed that keep her alive and healthy.
June, 18, is considered medically fragile due to a rare seizure disorder and cerebral palsy. That legal designation means she requires the highest level of medical care, all day every day, and qualifies for Medicaid to receive it.
Outside of a hospital and her home in Southeast Portland, there are few places equipped to provide it.
In a typical week, her parents, along with a team of nurses, help her breathe, eat and go to school. But sometimes, June needs more complex care after a hospital stay, or her parents need to go out of town.
Until recently, the Straceners felt fortunate to have the Providence Center for Medically Fragile Children nearby. It’s Oregon’s sole skilled nursing facility that is able to properly care for June, and it’s one of a handful of nursing facilities in the country created specifically for medically fragile children. In Oregon, the Department of Human Services’ Office of Developmental Disabilities provides case management for 111 children that it has determined are medically fragile, but the Providence center has also taken in children from Washington.
“It’s not my favorite thing for her to go there,” said June’s mom, Tina Stracener. “But I felt like she was very well cared for.”

A Hoyer lift installed on the ceiling of June Stracener’s bedroom plays a critical role in moving her safely between her wheelchair and her bed. Tina Stracener, her mother, left, operates the lift each day. (Leah Nash/InvestigateWest)
The Straceners, however, can’t place June at the facility anymore. Providence has closed the 58-bed Center for Medically Fragile Children to families seeking respite or short-term stays, even though its population of long-term residents is dwindling, too. Elderly patients who are not medically fragile have been moved into the larger of the center’s two floors, as the young residents are relegated to a smaller, less safe space, employees say. Staff and families fear the center will be shut down or be changed into an all-adult facility.
Providence told InvestigateWest that it has no plans to close the center but is adapting to Oregon’s policies that steer medically fragile children increasingly toward home and community-based services so they remain integrated in their families and neighborhoods.
“Serving medically fragile children is fundamental to our mission of caring for the poor and vulnerable,” said Jean Marks, spokesperson for Providence. “We are committed to serving our current residents with safe, compassionate care.”
Yet four current and former employees from the center told InvestigateWest that conditions inside the center have also worsened. The changes have medical staff raising alarms, including fears that remaining pediatric residents are being exposed to risk of infections and more acute medical crises.
Staff say they cannot isolate many of the remaining 17 long-term pediatric patients if one of them gets sick, because the second floor of the building has significantly less space. There, staff can only draw a curtain around most of the kids’ beds if they get sick, instead of isolating them to prevent the spread of infectious disease. And without access to the ceiling lifts installed on the first floor, lifting and moving children has also become more dangerous, they said.
While state policymakers and families prefer that medically fragile children get care outside of a hospital setting, some parents say the existing supply of home and community-based nursing and therapists is not enough to replace what the Providence center has provided for decades. Families continue to struggle to find nurses who can fulfill their hours allotted through Medicaid.
“We don’t have any safety net,” said Calli Ross, mother of a medically fragile 9-year-old and an advocate for families. “Every family I know is struggling. There isn’t a single family that has full hours being given to them.”
Changes spark staff concerns
In October 2022, staff at the children’s center received a message from Providence Portland Medical Center’s top executives announcing the expansion of intermediate care for adults at the center.
At the time, 23 young people were living there, all on the first floor. Chief Executive Krista Farnham and Kendall Sawa, chief operations officer, wrote that the children would be moved to the upper floor to prepare for the shift to adult care, according to a copy of the email reviewed by InvestigateWest.

June Stracener is one of 111 medically fragile children across Oregon, meaning she requires the highest level of continuous medical care to keep her healthy and safe. (Leah Nash/InvestigateWest)
The child center had housed adult patients temporarily before, taking in wildfire evacuees and discharged hospital patients during COVID-19 surges.
The decline in long-term pediatric residents is a result of changes in Oregon policy about where such children should find care, Providence leaders said. Children age out of the center after they turn 21, though some have been permitted to stay longer if there’s nowhere else suitable for them to go. But the state’s Office of Developmental Disabilities, which coordinates nursing and therapies for medically fragile children, favors services based in the home or local community over what it considers to be institutions and hospital settings such as the Providence center.
“The state has determined medically fragile children are best cared for in home and community-based settings and is no longer supporting long-term care admissions to our center,” said Farnham and Sawa in their message to employees.
InvestigateWest asked the Department of Human Services multiple times whether it makes any long-term care referrals to the Providence center, and what laws and policies guide the process. It did not provide any information.
But staff wondered if there was another motivation, especially as the center also began denying requests for respite care and step-down care for children after hospital visits.
“I can only assume it’s a money thing,” said Daisy Wright, who was the lead respiratory therapist for the center until this March. Because the adult patients are less medically complex, she said, “it seems like we can make more money in adult patients instead of children.”
The email announcing the changes came one month after Providence dissolved its Children’s Health Foundation, which managed philanthropic support for the children’s center. At the time, a form filed with the Oregon Department of Justice showed that assets “related to care of children at Providence Child Center” totaled $24.5 million. That included $16 million in endowment funds, according to the Children’s Health Foundation’s last IRS filing.
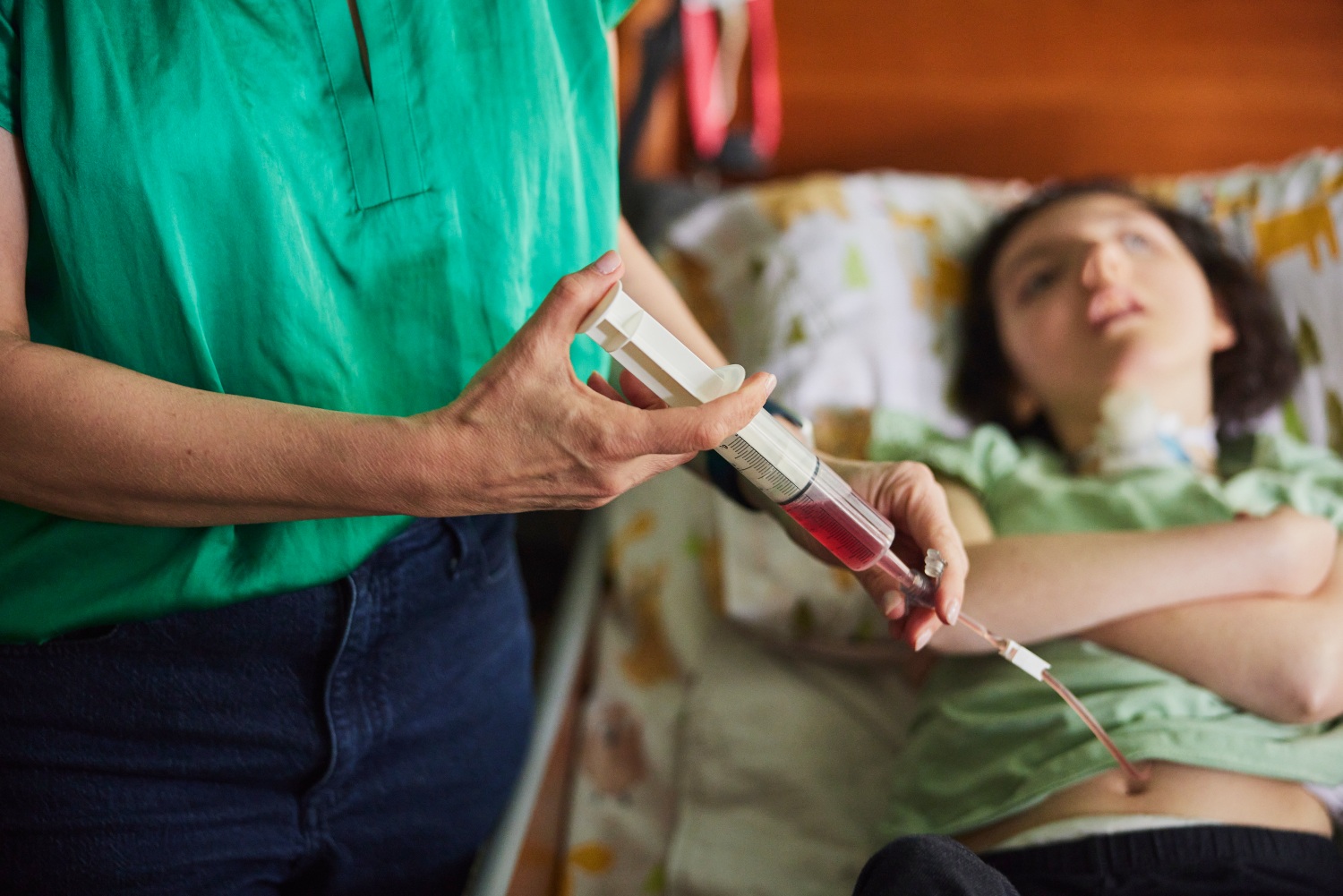
Tina Stracener administers food to her daughter June via a gastrostomy tube that connects straight to June’s stomach. (Leah Nash/InvestigateWest)
The Providence Oregon Board of Directors transferred philanthropic responsibility of the center to the Providence Portland Medical Foundation.
In addition to community support, Medicaid also helps pay for the care that medically fragile children receive at the center. But Providence is likely getting less of that money now that, according to its leaders, it’s not receiving long-term care referrals.
Without long-term residents, it’s not sustainable for the center to stay open to families primarily for respite or short-term care, said Marks, the Providence spokesperson.
“We staff and budget based on the number of long-term care residents we currently serve,” Marks said. “Respite and step-down care volume is fluid and not predictable, and therefore unreliable for staffing and budgeting purposes.”
Like many of Oregon’s hospital systems, Providence Health and Services is in a precarious spot financially, reporting a $1.2 billion operating loss across the multi-state system in 2023. Providence Portland Medical Center reported a 5.4% operating loss for the first three quarters of the year, The Lund Report reported in March.
Staff who spoke with InvestigateWest said that they still didn’t understand how the endowments tied to the center plus Medicaid aren’t enough to protect it from financial struggles even without long-term referrals. The dissolution of the children’s foundation, combined with other changes, made staff suspect that finances are driving the decisions at the children’s center, they said.
Wright, who was hired at the center in May 2020, said Providence was frequently not replacing her former colleagues when they quit. Respiratory therapists manage patients’ tracheostomies and ventilators, ensuring airways are clear and moisturized and preventing pneumonia from mucus buildup in the lungs.
Instead, Wright said, her boss asked her to train nurses to effectively replace respiratory therapists, a proposal she felt was insulting and unsafe.
“We were definitely sometimes dangerously short-staffed,” she said. Without respiratory therapists to monitor airways regularly and carefully, children are at higher risk for respiratory emergencies that can put them in the hospital, she said.
“It would (involve) an ambulance, a lot of resources,” she said. “The stress on their bodies … it affected them very negatively, I feel.”

Medical equipment including a ventilator, a cough assist machine and a mist machine are stored below June Stracener’s clothes in her closet. (Leah Nash/InvestigateWest)
Wright and three nurses who still work at the center and asked not to be named out of fear of retaliation also criticized Providence’s decision to shift the remaining pediatric patients into a smaller area of the center, characterizing it as a threat to patients’ safety.
They said the center implemented a new policy of “isolating at bedside” when a child comes down with an infectious disease, which can be particularly dangerous for medically fragile children. When the children were in the larger unit, staff could isolate them in a separate room, decreasing the likelihood that they would pass the illness on to others. By only drawing a curtain around sick children, staff worries that diseases will spread more easily.
One nurse said the center now doesn’t have enough electrical outlets to put ventilators in the right places, so the staff called a handyman to install power strips on the walls that aren’t hardwired in.
Other nurses said the lack of ceiling lifts is a major hazard. On a recent day, they said, the tracheostomy of a patient who depends on a ventilator to breathe fell out repeatedly when staff were trying to move him.
The nurses say supervisors have mostly brushed off their concerns.
“We’ve asked, ‘How are we supposed to transport this kid in the space you have given us?’” a nurse said. “No one will respond to us.”
Providence did not respond to InvestigateWest’s questions about the specific safety concerns of staff but stressed the center has the safety of patients in mind.
“We understand consolidating the space used for the facility is not ideal, but, of the options we have, we believe continuing to serve these families in some capacity is the best option,” Marks said.
Community services, but not enough
On a recent afternoon, Tina Stracener changes out the tube in June’s tracheostomy, the surgically created hole in her throat through which she breathes. This must happen once a month.
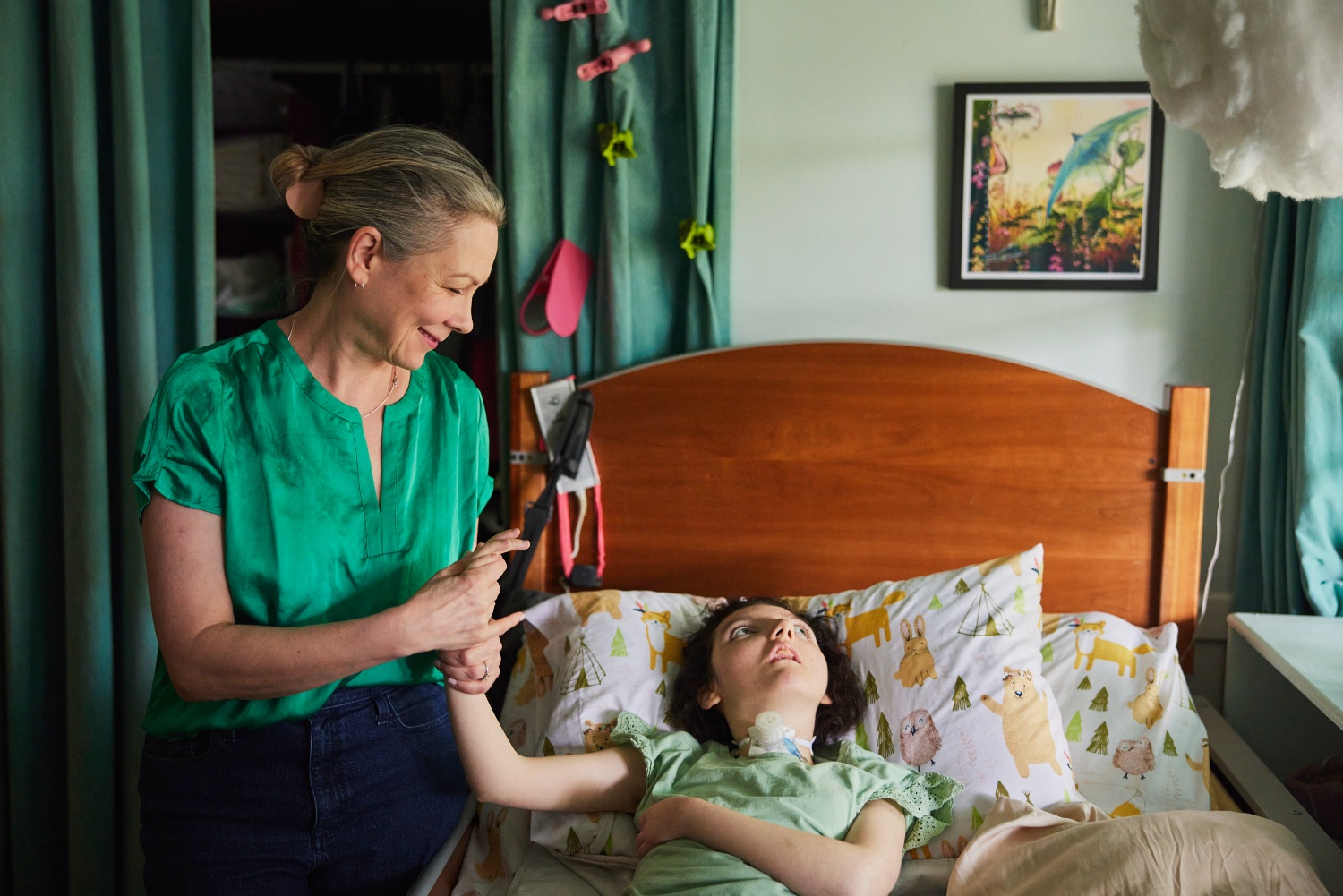
Tina and her daughter June Stracener in their Southeast Portland home on April 11, 2024. (Leah Nash/InvestigateWest)
A breathless moment unfolds as June’s oxygen level drops and a monitor beeps an alarm. But Tina, keeping calm, secures the mechanism and June’s oxygen level rises again.
“Not just anybody can do this,” Tina says.
Parents like her have learned to take on more and more of this kind of care in the home. Nationwide, the shift away from institution-based care came after a century of parents being pressured to turn children over for care outside of the home at medical or psychiatric facilities that were often poorly equipped to meet their needs and, in the worst cases, rife with abuse. The 1999 U.S. Supreme Court decision in Olmstead v. L.C. affirmed that states must provide community-based services to the greatest extent possible.
In Oregon, thousands of people with intellectual and developmental disabilities were sent to the Fairview Training Center, which operated east of Salem from 1908 until 2000. The darkest chapters of its legacy include forced lobotomies and sterilizations.
The Providence Center doesn’t share the same history as Fairview, but in the eyes of the state, it is still an institution, more like a hospital than a community-based resource such as a group home in a residential neighborhood.
“We want folks served in their home and in their community to the greatest extent possible,” said Alexis Alberti, head of the Multnomah County Intellectual and Developmental Disabilities Division, which refers families to services. “That doesn’t mean they can’t be served in a place like Providence, but the goal is always to get these individuals to home and community-based services.”
Not all parents agree that the Providence center is less of a community-based facility than others, however. Children who live there can attend school and leave with their families for outings.
Kristin Gurney, a parent in Vancouver whose son Jace has lived in the Providence center since 2019, said she has “really been impressed” with the center’s efforts to keep her son engaged in typical teen activities, including recently, shopping for an outfit for prom. A single mom, Gurney kept Jace at home for as long as she could before deciding the center was a better fit for his and her family’s needs.

June Stracener getting some fresh air outside their Southeast Portland home. (Leah Nash/InvestigateWest)
“I think there’s this big stigma around institutions,” she said. “My experience has been incredible, and that’s the only place I would want him.”
Additionally, parents said, the state lacks enough community programs and in-home nursing staff to meet families’ needs, particularly for respite care.
“Prior to COVID it was very difficult for anyone to get respite care,” said Ross. Now, she said, “I know so many people that are running on fumes. They have no services, they’re living off food stamps, taking care of vulnerable kids and terrified Child Protective Services is going to be called, but terrified to let incompetent workers into their home.”
So while the model of care the Providence center provides is no longer preferred, without it families and service providers don’t see an alternative.
“There will be a gap if the center closes,” said Alberti.
Even when families have home health nurses to fill the needs of their regular schedule, they need more nurses to accomplish respite care in the home. Families also need to cobble together additional caretakers to give nurses their required breaks.

Tina Stracener adjusts her daughter June’s percussive vest, which uses oscillations to keep her airways clear and moisturized. June, 18, who has cerebral palsy and a rare seizure disorder, requires round-the-clock, hospital-level care. (Leah Nash/InvestigateWest)
June Stracener’s parents can manage some form of respite care with a combination of June’s home health nurse, grandmother and older sister. If all goes well, it’s enough to get the couple just a day or two away.
Even then, Tina said, “It’s anxiety-provoking. Because if a nurse doesn’t show up for a shift, that’s too much on my mother.”
Without the Providence center to care for June, their family is out of options for any longer break.
“They’re the only game in town,” she said. “There is no other thing.”
FEATURED IMAGE: Tina and her daughter June Stracener in their Southeast Portland home on April 11, 2024. (Leah Nash/InvestigateWest)
InvestigateWest (invw.org) is an independent news nonprofit dedicated to investigative journalism in the Pacific Northwest. Reach reporter Kaylee Tornay at kaylee@invw.org.



